Key Points
- Manual therapy combined with specific exercise is more effective than dry needling with exercise in reducing pain and improving function in people with mechanical neck pain.
- Multimodal physical therapy approaches consistently produce better outcomes for mechanical neck pain compared to single treatments alone.
- Clinical implication: Physiotherapists should consider manual therapy plus exercise as the preferred option for treating mechanical neck pain, whilst recognising short-term gains from dry needling.
- Study limitation: Only mechanical neck pain was studied; findings may not apply to other neck pain types or different manual therapy or dry needling methods.
- Patient implication: Patients can expect greater and longer-lasting relief from a programme that combines manual therapy and exercises, rather than dry needling alone.
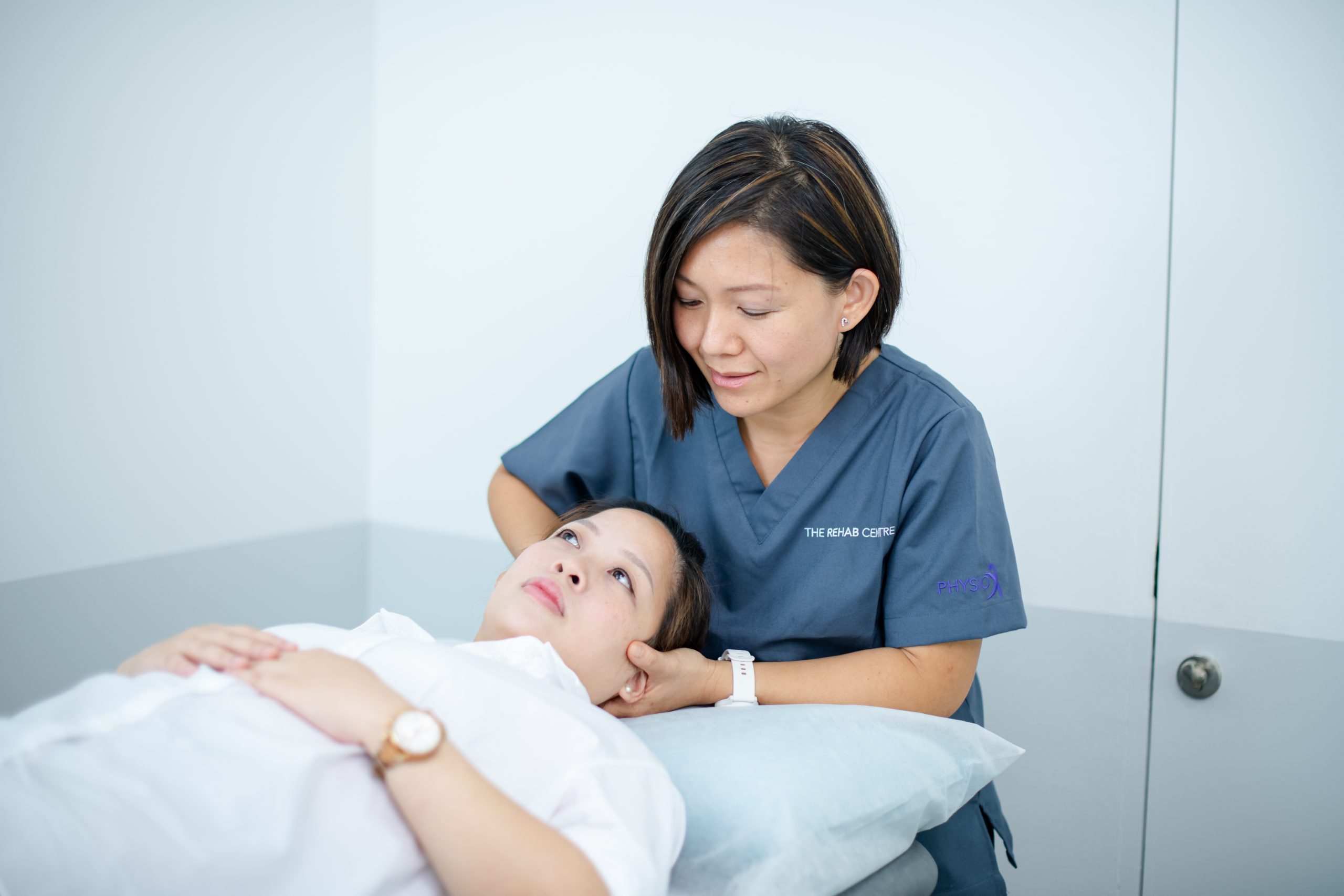
Understanding Mechanical Neck Pain
Neck pain is a very common health concern that can affect anyone. Surveys show 20% to 70% of people will experience neck pain at least once in their lives. This problem strikes people of all ages, although it is particularly frequent in women, individuals living in cities, and those aged between 35 and 50. It can have a substantial physical, social, psychological, and financial impact—affecting not only the person but also their families and communities. In Singapore, as in the rest of the world, people frequently seek physiotherapy to help manage their neck pain and restore their quality of life.
Mechanical neck pain is the focus of the randomised controlled trial discussed here. This type is defined as pain located in the neck, intermittent or constant, which does not radiate below the shoulder and is not due to nerve root issues or major underlying conditions. The point prevalence can range widely—from 6% to almost 39% of people—especially increasing in those older than 65.
Many factors can contribute to developing neck pain. These range from ergonomics and posture to psychological and behavioural issues. For some, work at a desk or long periods at a computer are triggers. For others, life stresses, low mood, and worry about pain contribute to the problem. Physiotherapists appreciate this complexity and seek to offer evidence-based treatments that deliver both pain relief and improvements in daily activity.
Current Approaches To Treating Mechanical Neck Pain
Traditionally, there have been many recommended approaches to non-surgical management of neck pain. Popular strategies include patient education, exercise, spinal mobilisation and manipulation, massage, dry needling, and various electrotherapy techniques. Recent international guidelines recommend that the best outcomes come from blending multiple treatments. This means using, for example, a programme that combines manual therapy or dry needling with individually tailored exercise.
However, there has been uncertainty over which combination works best. The American clinical practice guidelines support both manual therapy and dry needling in conjunction with cervical and scapulothoracic exercises. Still, the critical question remains—should manual therapy or dry needling take priority, or do they provide similar results when combined with exercise?
This blog reviews the meaningful results of a high-quality randomised trial carefully designed to answer this question.
Summary Of The Research Study
Seventy-eight people living with mechanical neck pain were recruited and randomly assigned to one of two treatment groups:
- Dry Needling plus Therapeutic Exercise (DN + Exercises)
- Manual Therapy plus Therapeutic Exercise (MT + Exercises)
Participants were average 51 years of age. Both groups attended seven half-hour treatment sessions over up to six weeks. The main question was: Which combination leads to more reduction in pain, more improvement in daily function, and higher patient satisfaction?
Outcomes measured included:
- Neck Disability Index (NDI): Assesses neck-related disability
- Pain Scores (NPRS): Rates severity of neck pain
- Patient-Specific Functional Scale (PSFS): Evaluates ability to perform daily tasks
- Fear-Avoidance Belief Questionnaire (FABQ): Checks beliefs about pain and movement
- Deep Neck Flexor Endurance Test (DNFET): Measures neck muscle endurance
- Global Rating of Change (GROC): Patient’s own view of improvement
Outcomes were tracked at the start, two weeks, at the end of the course (after session seven), and three months following discharge.
Details Of The Treatments Provided
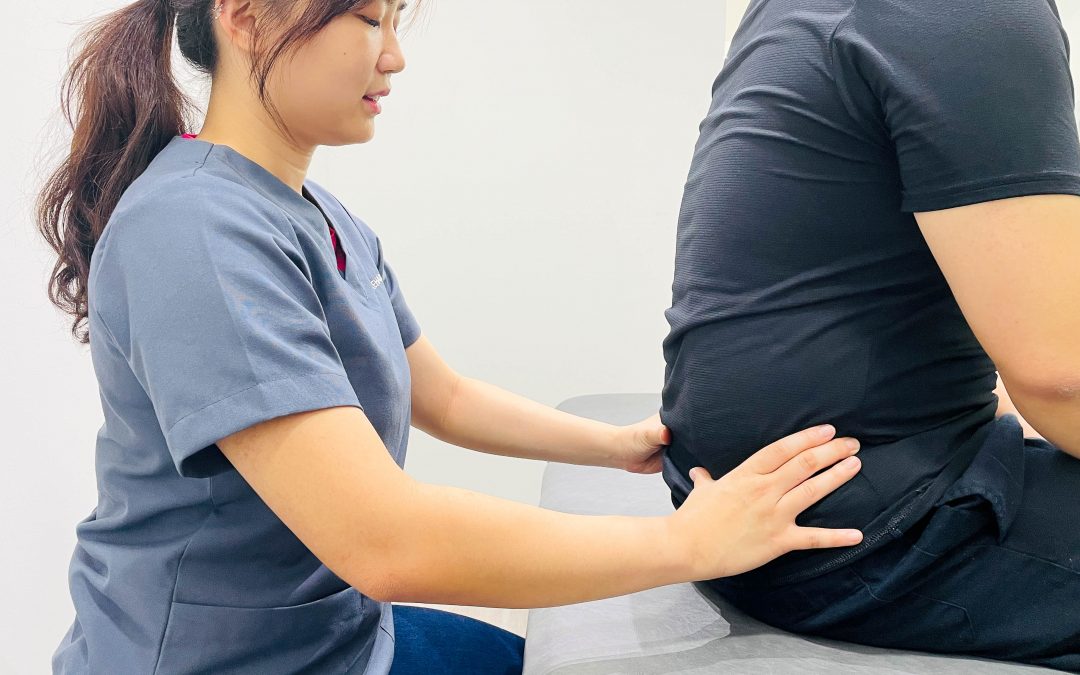
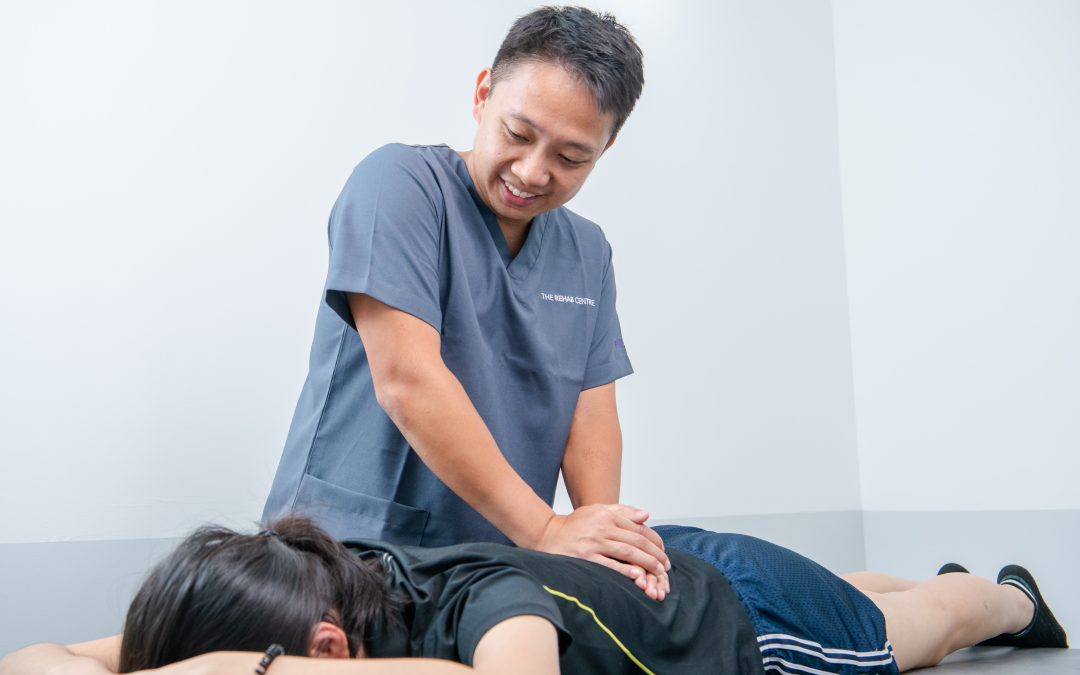
Manual Therapy (MT):
Participants in the MT group received hands-on joint mobilisation and manipulation techniques for the cervical and upper thoracic spine (including targeted thrust and non-thrust techniques), combined with five prescribed exercises. The specific manual techniques addressed movement restrictions and aimed to modulate pain and improve neck mobility.
Dry Needling (DN):
Participants in the DN group received dry needling of the main muscles at the back of the neck and upper back where myofascial trigger points were identified. Up to 20 trigger points could be targeted during a session. This was followed by the same set of prescribed exercises as the manual therapy group.
Therapeutic Exercise:
Both groups completed exercises targeting strength and flexibility for the cervical spine, thoracic spine, and the scapular region. The five prescribed exercises included:
- Supine deep neck flexor strengthening
- Active range of motion for cervical rotation
- Seated upper trapezius stretch
- Prone middle trapezius strengthening
- Prone lower trapezius strengthening
All received a home exercise diary with visuals. Usual activity was maintained within pain limits.
Results: Which Treatment Was More Effective?
Main Outcome: Disability Reduction
Manual therapy with exercises was consistently more effective at reducing neck pain disability than dry needling with exercises. The advantage was present at every measured stage—two weeks, after all sessions, and even three months after treatment concluded.
- Neck Disability Index (NDI): The manual therapy group had much greater and clinically meaningful reductions in neck disability, both immediately and three months down the line.
Pain Relief
Individuals in the manual therapy group experienced both bigger initial and sustained improvements in pain scores. Greater reductions in pain (measured on the numeric pain-rating scale) were achieved and the effect lasted to the three-month follow-up.
Functional Improvement
Manual therapy with exercise led to more noticeable gains in function (measured by the PSFS). People were able to do more of their day-to-day tasks, with less restriction and discomfort.
Beliefs And Fear About Movement
Both groups improved, but the manual therapy group showed bigger decreases in fear of pain and avoidance of activity (measured by FABQ). Changing beliefs about movement is important for long-term recovery and confidence.
Endurance And Muscle Strength
Both groups improved in deep neck flexor endurance in the early phase, but the gains were not significant at three months.
Patient Global Assessment And Satisfaction
The global rating of change—how much better patients felt overall—was substantially higher in the manual therapy with exercise group. In fact, by three months, over 87% of discharge patients said they felt much improved with manual therapy, compared to about 53% in the dry needling group.
Adverse Events
No major adverse events occurred in either group. Minor short-lived soreness or discomfort was more common after dry needling. Examples included pain during the procedure or soreness that faded within 24–48 hours. Manual therapy also had minor side effects, but these were less frequent.
Understanding These Results In Practice
These findings support a modern trend in physiotherapy—using multimodal approaches, especially combining manual therapy with well-chosen exercises, leads to the best results for most people with mechanical neck pain. This approach provides both faster and more sustained relief compared to dry needling plus exercise.
Manual therapy worked particularly well for reducing disability and pain, improving daily function, and leading to overall patient satisfaction, both in the short and medium term. Notably, dry needling did deliver some improvement, especially for short-term pain, but its effects were not as long-lasting or marked.
Why Not Just Use Exercise Alone?
Some may wonder whether exercise alone is just as useful. Earlier research has shown that while exercise is helpful (and should always be part of any programme), it is when it is combined with carefully selected manual approaches that patients see the largest, and most rapid, improvements. Neither manual therapy nor dry needling alone is typically enough for full recovery—multimodal therapy is the preferred strategy in all major guidelines for mechanical neck pain.
Clinical Implication
The evidence is now clear that manual therapy combined with specific exercises should be the preferred initial strategy for people with mechanical neck pain. While dry needling plus exercise can be considered for selected patients, particularly in the very early stages where quick pain relief is wanted, it does not match the effectiveness of manual therapy for medium-term and sustained outcomes. These results align with recommendations from the leading clinical guidelines worldwide.
Study Limitation
It is important to note that this study focused solely on mechanical neck pain. Patients with nerve root symptoms, radiating pain below the shoulder, or systemic conditions were excluded. This means the results cannot necessarily be applied to other types of neck pain or other populations. There was also no blinding of the treating therapists or patients—a potential source of response bias. Different manual therapy or dry needling techniques or treating different muscle groups may lead to other findings. Moreover, compliance with home exercise diaries, though encouraged, was not rigorously measured.
Patient Implication
For those living with neck pain, these findings are highly relevant. Patients can feel reassured that the combination of manual therapy and exercise offers not just short-term but also sustained benefits. This approach was more likely to restore your function, reduce your pain, and keep you feeling better three months and beyond. In contrast, dry needling—whilst generally safe and able to provide brief relief—did not maintain the same gains in pain or function. If you are searching for long-lasting improvement, a physiotherapy programme focused on manual therapy with exercise is likely your best pathway.
Is Dry Needling Helpful In People With Neck Pain?
Many people ask whether dry needling is a worthwhile treatment for neck pain. The latest research provides some answers.
Dry needling involves inserting thin needles into myofascial trigger points within neck and upper back muscles. This treatment can sometimes offer short-term relief of pain or discomfort by targeting areas of tightness and sensitivity. In the study discussed here, people who received dry needling with specific exercises experienced some improvement in pain and daily function, especially in the short term. Most participants tolerated the procedure well, with only minor and brief side effects like temporary soreness or pain during the session.
However, the benefits of dry needling for neck pain were generally less strong and did not last as long as those seen with manual therapy plus exercise. At three months after finishing therapy, the manual therapy group had less pain, less disability, and reported better overall progress than the dry needling group. The research suggests that while dry needling may be a reasonable option—especially for quick pain relief early in care—it is not sufficient by itself for lasting results. It works best as part of a well-structured, comprehensive physiotherapy plan.
Therefore, dry needling can be helpful for neck pain, but better results are usually achieved when manual therapy and targeted exercise form the core of your programme.
References
Pandya, J., Puentedura, E. J., Koppenhaver, S., & Cleland, J. (2024). Dry Needling Versus Manual Therapy for Patients With Mechanical Neck Pain: A Randomized Controlled Trial. Journal of Orthopaedic & Sports Physical Therapy, 54(4), 267–278. https://doi.org/10.2519/jospt.2024.12091